External Iliac Artery Transection Managed by Iliofemoral Bypass Grafting Using Temporary Balloon Occlusion
Article information
Abstract
Traumatic abdominal vessel injury is rare, but difficult to manage. Approaching the injured vessel and controlling the bleeding is very hard. We experienced the right iliac artery transection managed by iliofemoral bypass grafting using temporary balloon occlusion. Proximal occlusion of an iliac artery with a temporary balloon cab be an option or bridge technique for a definite operation in case of iliac artery rupture. So, we present our case.
INTRODUCTION
Traumatic abdominal vessel injury is rare, lethal and difficult to manage. The mortality rate of abdominal vessel injuries is as high as 20–60%, with early death occurring due to bleeding and later deaths resulting from multi-organ failure [1]. In arterial injuries, early resuscitation and bleeding control are the most important principles and both of them must be accomplished at the same time. Interventions like temporary ballooning or bypass grafting during operations can be used as controlling techniques.
We experienced a traumatic external iliac artery transection case controlled by a temporary ballooning of the common iliac artery with an endovascular procedure and iliofemoral bypass grafting. This report describes the details of that case.
CASE REPORT
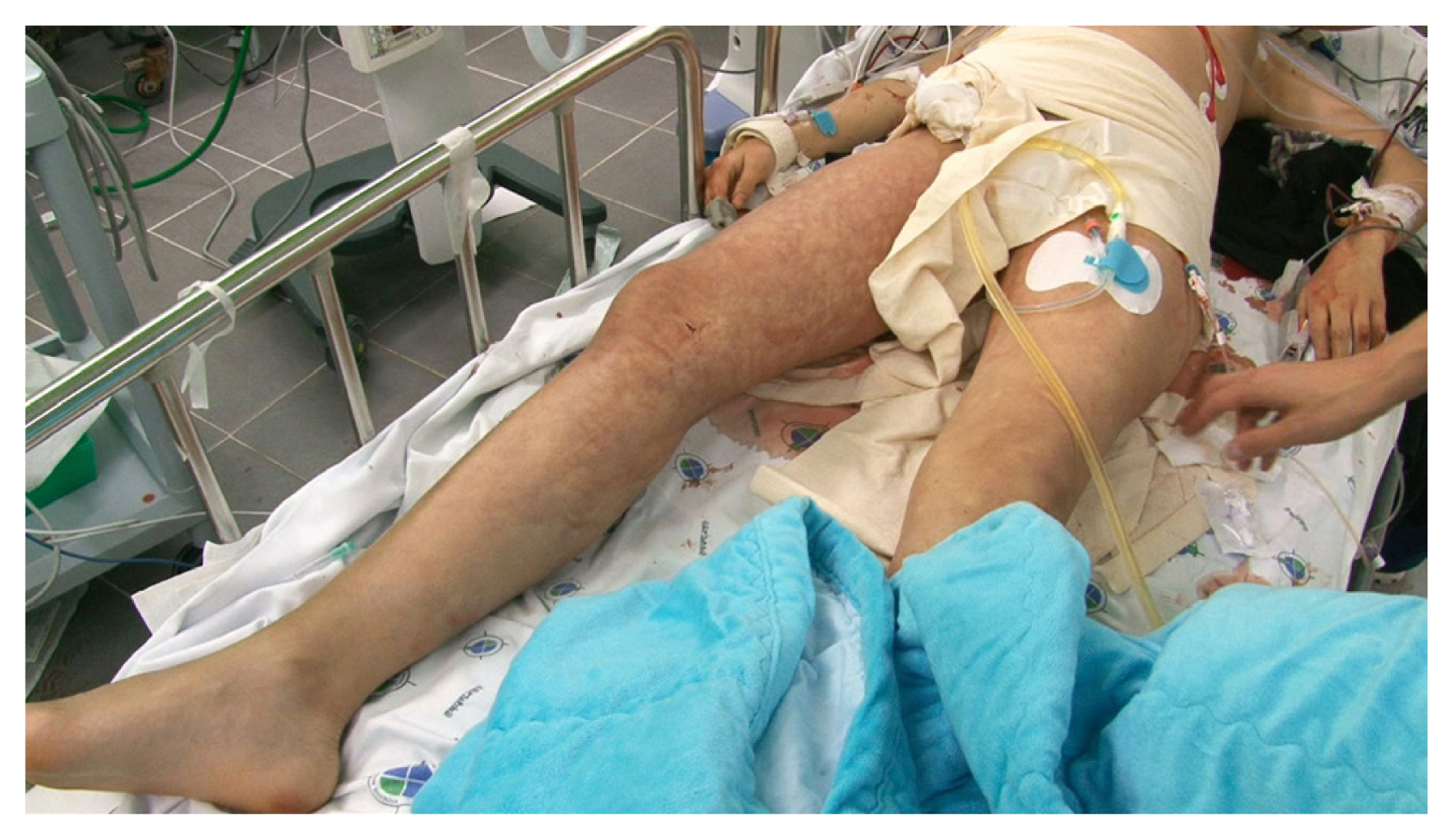
A 12-year-old girl was transferred to the emergency department of a hospital for retroperitoneal hemorrhage. The interval time from the accident to the emergency department (ED) was 167 minutes. She had an injury on her lower abdomen from a bicycle handle. Upon arriving at the hospital, her vital signs were stable and hemoglobin level was 10.6 g/dL. Abdominopelvic computed tomography scan displayed a large amount of hemorrhagic fluid collected at the right retroperitoneal space and anterior abdominal wall with active bleeding (Fig. 1). However, after being transferred to the emergency department, her hemoglobin level went down to 6.7 g/dL and blood pressure was 142/88 mmHg with a pulse rate of 102 beats per minute. Her right leg exhibited a grossly acute limb ischemia pattern (Fig. 2).
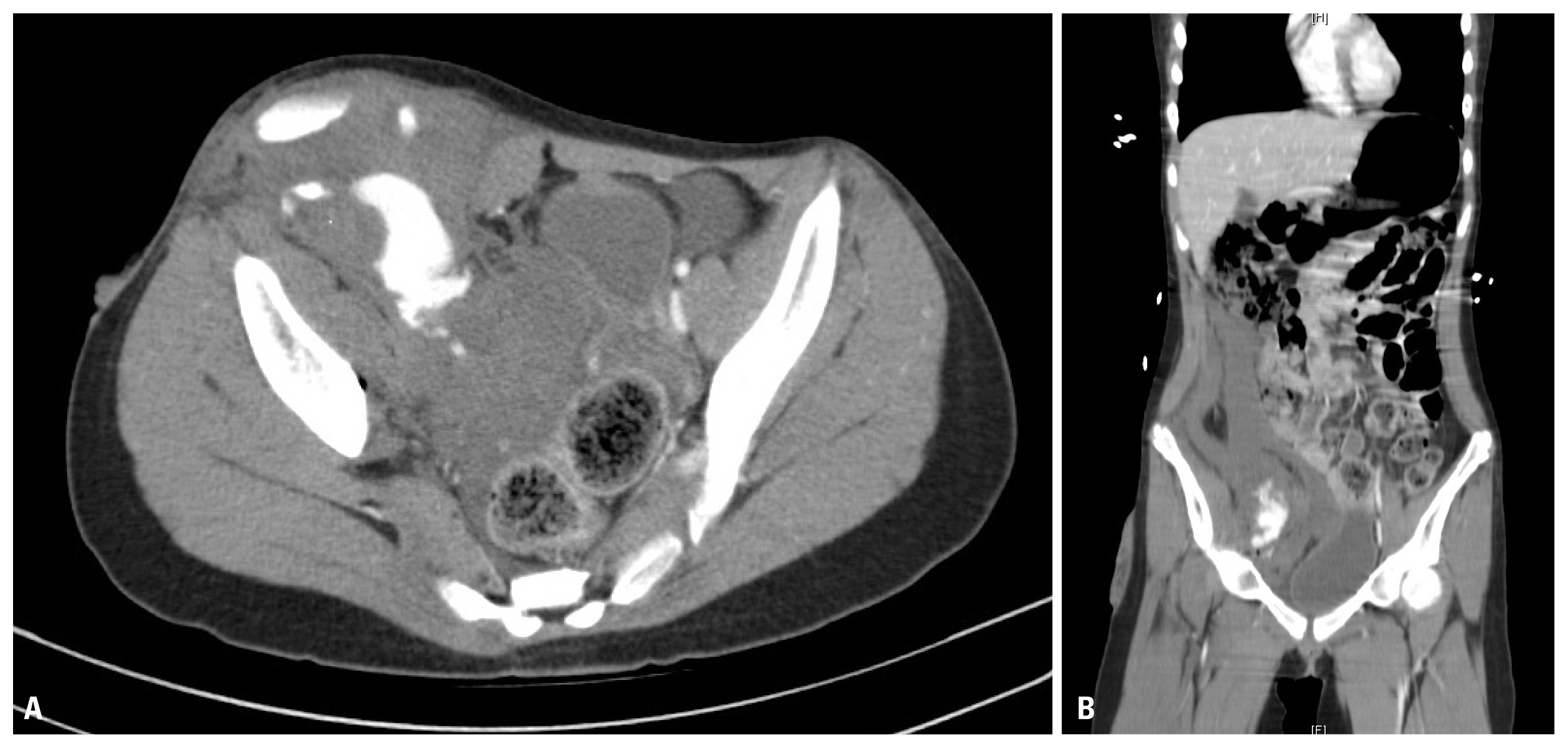
(A) Preoperative abdominopelvic computed tomography showing a large amount of hemorrhagic fluid collected at the right extraperitoneal space and anterior abdominal wall with active bleeding. (B) On coronal view.
An emergency operation was decided and the patient was sent to operation room with a transfusion. For bleeding control, an angiography with a ballooning occlusion was considered before surgery. An angiocatheter was inserted into the left femoral artery and an angiography was conducted with a portable X-ray (C-arm). This procedure was done by a cardiologist. The discontinuation of the right common iliac artery was checked and temporary occlusion with ballooning of the right common iliac artery was performed. Then, hockey-stick incision was applied to approach retroperitoneal space, however there was a severe bowel edema. Therefore, we used a transperitoneal approach with right-sided paramedian incision of the abdomen. After evacuation of the hematoma, a transection of the right external iliac artery was found, not common iliac artery, and the proximal and distal parts were isolated. Right iliofemoral bypass grafting with polytetrafluroroethylene was applied. The abdomen became distended due to bowel edema during the operation and the temporary abdominal closure technique with a vacuum pack was performed to protect against abdominal compartment syndrome. After the operation, the patient was moved to the trauma intensive care unit with an intubated status and her vital signs were stable. On postoperative day (POD) 3, the open abdomen was closed in the operation room and extubated the next day. On POD 5, she was transferred to the general ward. An electrophysiologic study on POD 16 displayed an incomplete lesion in the peroneal component of the sciatic nerve at or below the gluteal fold level. She was transferred to the rehabilitation department for gait training with completion of wound management on POD 25. On a manual muscle test, motor power weakness of the right lower extremity with a poor to fair grade improved to a good and fair grade 24 days after transferring. Moreover, the right foot drop with a poor grade of dorsiflexor motor power checked when gaiting was improved with the application of an ankle foot orthotic and gait training. On POD 50, she was discharged and no new or worsening of complications occurred.
DISCUSSION
In all vascular injuries, the time it takes to control proximal and distal bleeding is the most important factor in predicting outcomes [2]. There are several strategies to control abdominal bleeding. However, massive bleeding interferes with the approach to the bleeding site which frustrates surgeons. Intraabdominal packing is the usual method for venous or oozing bleeding [3]; however, it is not effective for controlling arterial bleeding.
For massive abdominal hemorrhages, an aortic cross clamping (ACC) can be a bridge technique for definitive operations. As the ACC separates systemic circulation from the outflow of the heart, bleeding control from the main vessel including ligation or a bypass graft would be easier. Yet, the ACC technique is hard to achieve in situations accompanied by severe bleeding and there are still no concrete guidelines and protocols for performing the procedure.
Another option for a massive abdominal hemorrhage is resuscitative endovascular balloon occlusion of the aorta (REBOA) [4]. It places an endovascular balloon into the aorta to stop bleeding or control blood flow distal to the balloon in hypovolemic shock and traumatic arrest states [5]. In 1954, Hughes [6] reported the use of an intra-aortic balloon catheter tamponade for controlling intraabdominal hemorrhage in men and in 1989, Gupta et al. [7] discussed the role of an intra-aortic balloon occlusion in penetrating abdominal trauma. Avaro et al. [8] reported that an endovascular aortic occlusion that is performed in forty minutes increases the survival rate in an experimental model of hemorrhagic shock by abdominal trauma. It is clear that the REBOA procedure keeps the perfusion to the heart and brain so that hypovolemic shock can be avoided for a short period of time. However, this procedure can be a bridge skill to move patients in poor conditions from the emergency department or intensive care unit to the operating or angiography room [9]. In 2017, a consensus was obtained at a meeting held in Sweden. Since the procedure was just recently established, its effectiveness is now being announced in several small studies and its indications are being set. Even though its indications are different depending on the country and hospital, it is typically used in hemorrhagic shock, blunt or penetrating abdominal trauma, hemorrhagic pelvic bone fracture, and aneurysmal rupture of the abdominal aorta in patients who are in or about to arrest. However, the crucial complication of REBOA is the ischemia such as limb amputation and organ failure which is as high as 13% [10]. For a more clear and improved option than aortic clamping, more studies with hemorrhage-related mortality are needed [5].
Iliac vascular injuries represent 11% of cardiovascular injuries, and 26% of those have combined injuries such as a pelvic bone fracture and internal organ injuries [11,12]. An iliac vascular injury can cause a massive hemorrhage and result in hypovolemic shock. The mortality rate ranges from 42–58% when accompanied by an aorta or inferior vena cava injury [2]. For surgical management, an end-to-end anastomosis with appropriate mobilization can be applied to large vessel injuries. Moreover, polytetrafluoroethylene bypass grafting or saphenous vein interposition grafting can be applied when adequate mobilization cannot be achieved. However, the operative approach to retroperitoneum and vascular exposure is relatively difficult and requires a significant amount of time. Moreover, a blind dissection to large vessels in the retroperitoneum can cause unintended vessel or nerve injuries. Therefore, other options should be considered. The shunt can be used for temporary distal circulation in iliac artery injuries.
Martinelli et al. [13] reported that a blinded intra-aortic balloon occlusion procedure can help critically ill patients with refractory hemorrhagic shock due to a pelvic bone fracture. It can be a bridge strategy until the injured vessel is exposed. Radiologic embolization of an internal iliac artery or its branches is commonly used in a pelvic bone fracture [14]. For non-operative management, an endovascular balloon can also help control hemorrhages and facilitate selective occlusion of an injured point.
In our case, the rupture of the right external iliac artery caused massive bleeding and a large hematoma at the extraperitoneal and intraperitoneal spaces. Temporary occlusion with a balloon was applied to control bleeding after the angiography. This procedure had many advantages in this situation. First, it temporary clamped the arterial bleeding site and a clear operation view was secured. Second, since the procedure involved a highly selective occlusion, unnecessary organ ischemia was avoided. This point makes this procedure a better option than REBOA. Third, it was a temporary procedure that allowed the reperfusion to follow thereafter, which is better than angioembolization. Fourth, the procedure can be applied to large arteries, which can be difficult in the embolization process. Fifth, since the procedure was being performed at the same time as the operation, it saved time.
However there can also be disadvantages. First, the routine appliance of REBOA is not easy and the appliance can be considered case by case. Second, this procedure needs a highly selective angiography, therefore the expert and equipments of angiography are needed. In the future, we need a prospective study about the effectiveness of temporary ballooning of an artery in the trauma field.
In conclusion, the proximal occlusion of an iliac artery with a temporary balloon is an option or bridge for a definite operation in cases of iliac artery rupture.