Articles
- Page Path
- HOME > J Trauma Inj > Volume 35(Suppl 1); 2022 > Article
-
Case Report
Portal vein embolization in intrahepatic portal vein injury after blunt trauma: a case report -
Sung Hoon Cho, MD1,2
 , Sang Yub Lee, MD3
, Sang Yub Lee, MD3 , Jung Geun Cha, MD3
, Jung Geun Cha, MD3 , Jihoon Hong, MD3
, Jihoon Hong, MD3 , Sangcjeol Lee, MD1,4
, Sangcjeol Lee, MD1,4 , Kyoung Hoon Lim, MD1,2
, Kyoung Hoon Lim, MD1,2
-
Journal of Trauma and Injury 2022;35(Suppl 1):S31-S34.
DOI: https://doi.org/10.20408/jti.2022.0013
Published online: May 19, 2022
- 2,363 Views
- 56 Download
- 1 Crossref
1Trauma Center, Kyungpook National University Hospital, School of Medicine, Kyungpook National University, Daegu, Korea
2Department of Surgery, Kyungpook National University Hospital, School of Medicine, Kyungpook National University, Daegu, Korea
3Department of Radiology, Kyungpook National University Hospital, School of Medicine, Kyungpook National University, Daegu, Korea
4Department of Thoracic and Cardiovascular Surgery, Kyungpook National University Hospital, School of Medicine, Kyungpook National University, Daegu, Korea
- Correspondence to Kyoung Hoon Lim, MD Department of Surgery, Kyungpook National University Hospital, 130 Dongduk-ro, Jung-gu, Daegu, 41944, Korea Tel: +82-053-420-5605 E-mail: drlimkh@knu.ac.kr
Copyright © 2022 The Korean Society of Traumatology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Mortality from hepatic injury has declined over the last several decades for various reasons, including nonoperative management, such as angioembolization, in more than 80% of cases. Conversely, surgical treatment is preferred in intrahepatic portal vein injury due to several reasons. Here, we report a case that treatment of blunt traumatic liver injury accompanied by intrahepatic portal vein injury through portal vein embolization. A 29-year-old female patient was transferred to our trauma center for vehicular accident injuries. Contrast-enhanced abdominal computed tomography showed a massive hemoperitoneum and liver laceration (grade IV) with contrast extravasation suspected of the right portal vein branch but no other organ injury. Since vital signs were stable, we decided to perform nonsurgical radiologic intervention. Portography showed active bleeding of the posterior branch of the right portal vein. A pseudoaneurysm in the portal vein was embolized through percutaneous transhepatic portal vein puncture. On follow-up liver dynamic computed tomography performed 2 days after embolization, the posterior branch of the right portal vein was sufficiently embolized, and no liver parenchymal necrosis was observed. The patient was discharged without any complications 2 weeks later. This report suggests portal vein embolization as a good alternative treatment method for portal vein injury in patients with stable vital signs.
- The liver is the most frequently injured abdominal organ following abdominal trauma. Fortunately, mortality from hepatic injury has declined over the past several decades for various reasons, including the evolution to the current approach of nonoperative management of hepatic trauma in more than 80% of cases [1]. Conversely, surgical treatment is preferred in intrahepatic portal vein injury due to several reasons. This report describes the nonsurgical treatment of a case involving blunt traumatic liver injury accompanied by intrahepatic portal vein injury through portal vein embolization (PVE) and establishes the characteristics of intrahepatic portal vein injury and indications for PVE. The patient provided informed consent for publication of the research details and clinical images.
INTRODUCTION
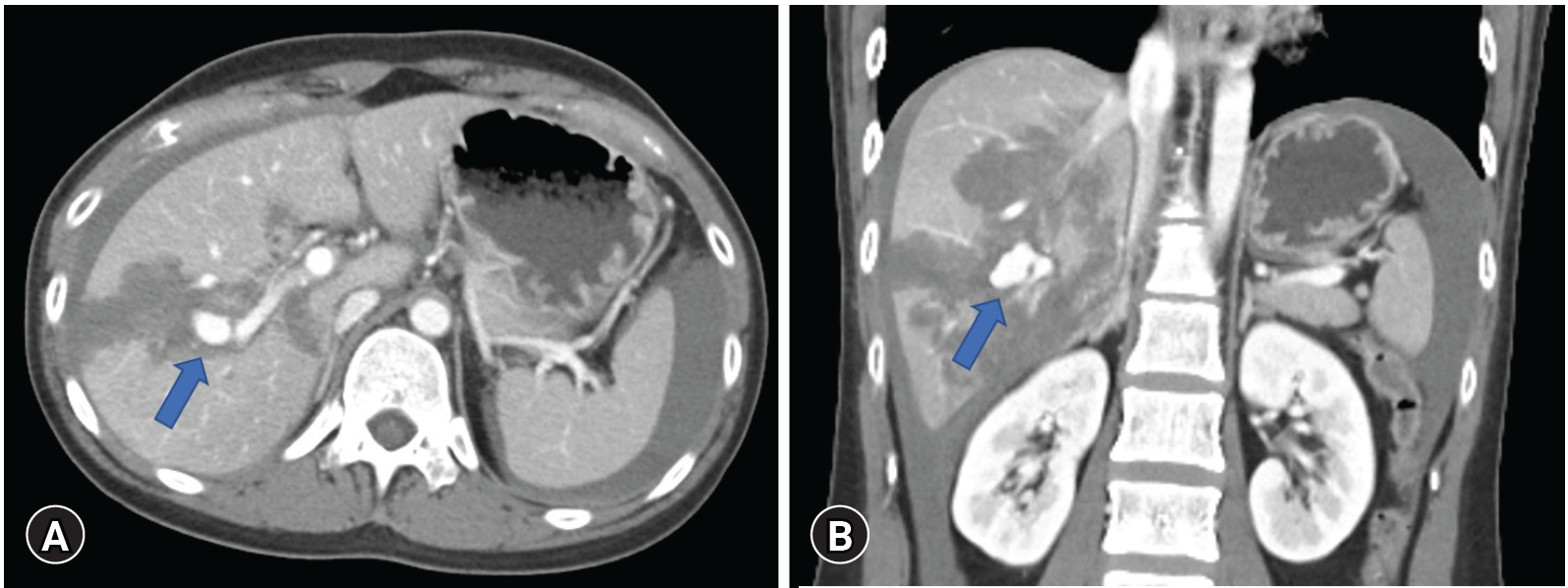
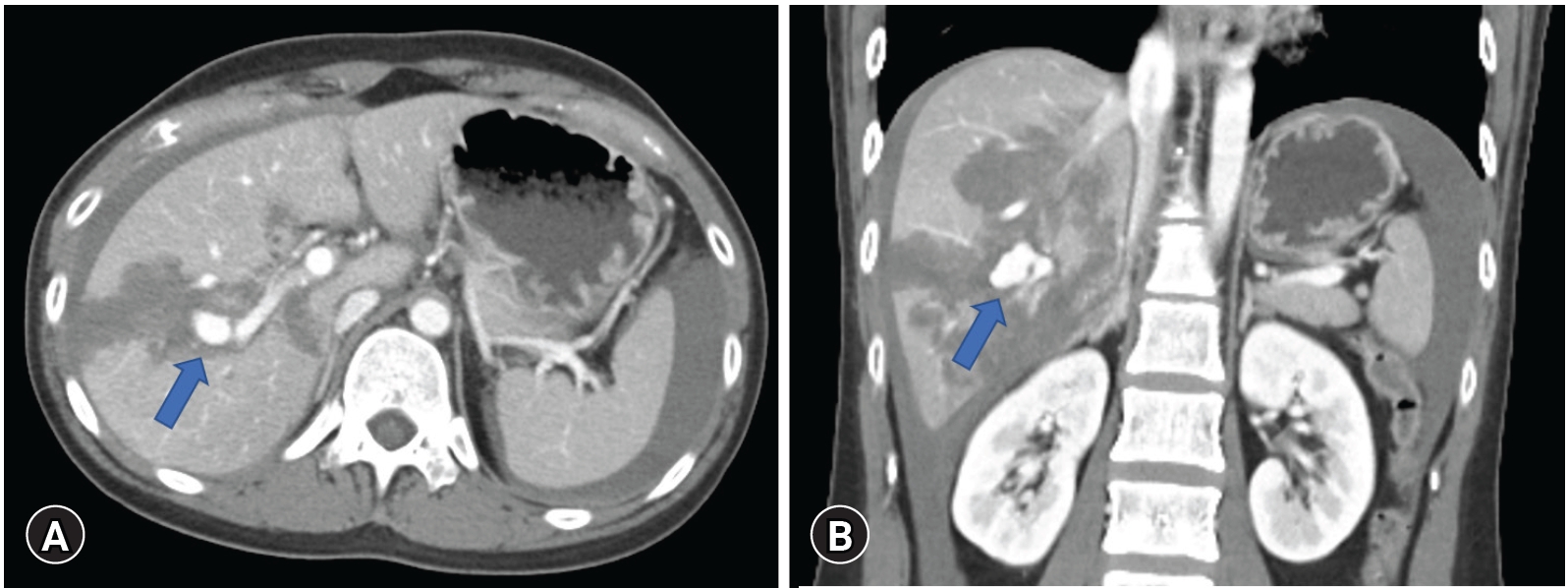
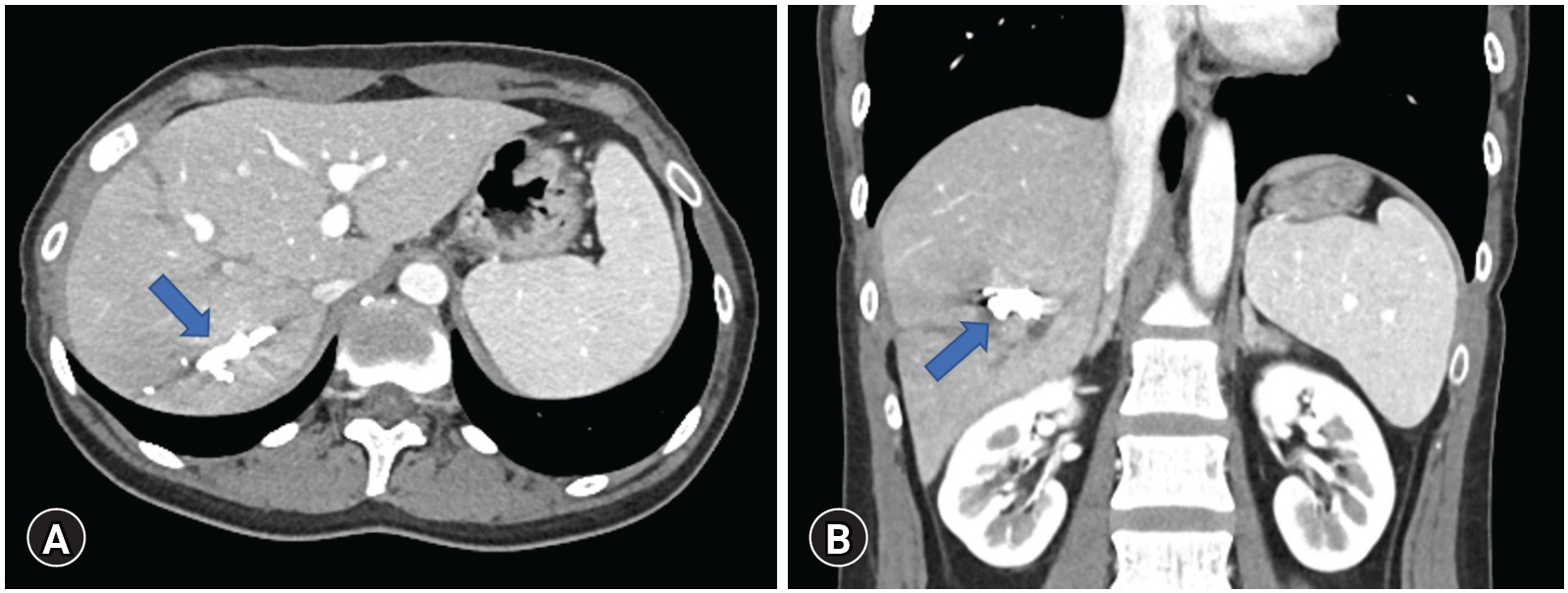
- A 29-year-old female patient with no medical history was transferred to the Trauma Center of Kyungpook National University Hospital for injuries sustained after a passenger car accident. Her initial blood pressure was 115/81 mmHg and heart rate was 112 beats/min. Hemoglobin and platelet count was 14.3 g/dL and 190,000 /µL, respectively. Contrast-enhanced abdominal computed tomography showed a massive hemoperitoneum and liver laceration (grade IV) with contrast extravasation suspected of the right portal vein branch, but no other organ injury (Fig. 1).
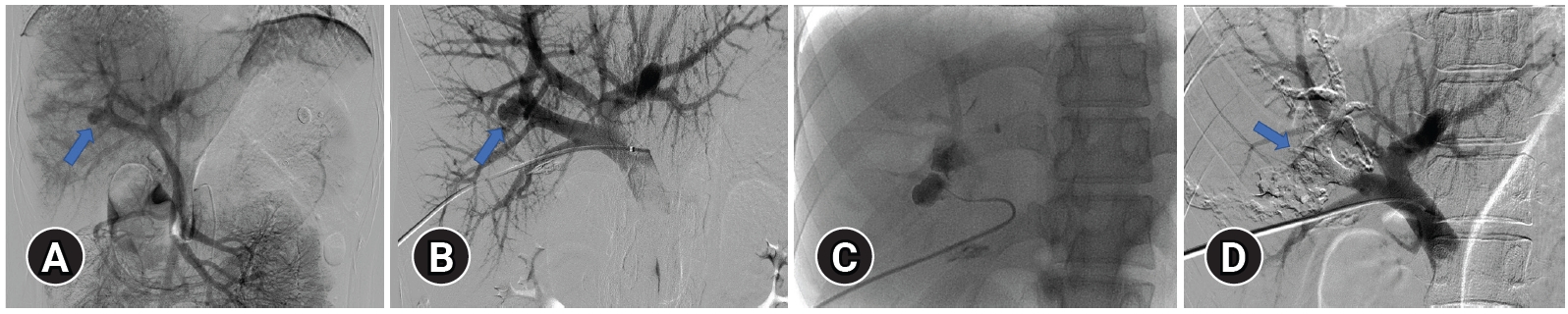
- Since the patient’s vital signs were stable, we decided to perform nonsurgical radiologic intervention rather than surgery. The celiac artery angiography did not show active bleeding of the hepatic artery branch, but portography following superior mesenteric artery angiography showed a pseudoaneurysm in the posterior branch of the right portal vein (Fig. 2A). An angiography sheath was inserted through the P5 portal vein branch by percutaneous transhepatic approach to access the proximal portion rather than the injured portal vein branch, and portography showed a pseudoaneurysm at the proximal portion in posterior branch of right portal vein (Fig. 2B, C). The pseudoaneurysm was embolized using a mixture of glue (Histoacryl; B. Braun, Melsungen, Germany) and lipiodol (Lipiodol Ultra-Fluid; Guerbet, Villepinte, France). Portography performed after the procedure no longer showed active bleeding (Fig. 2D).
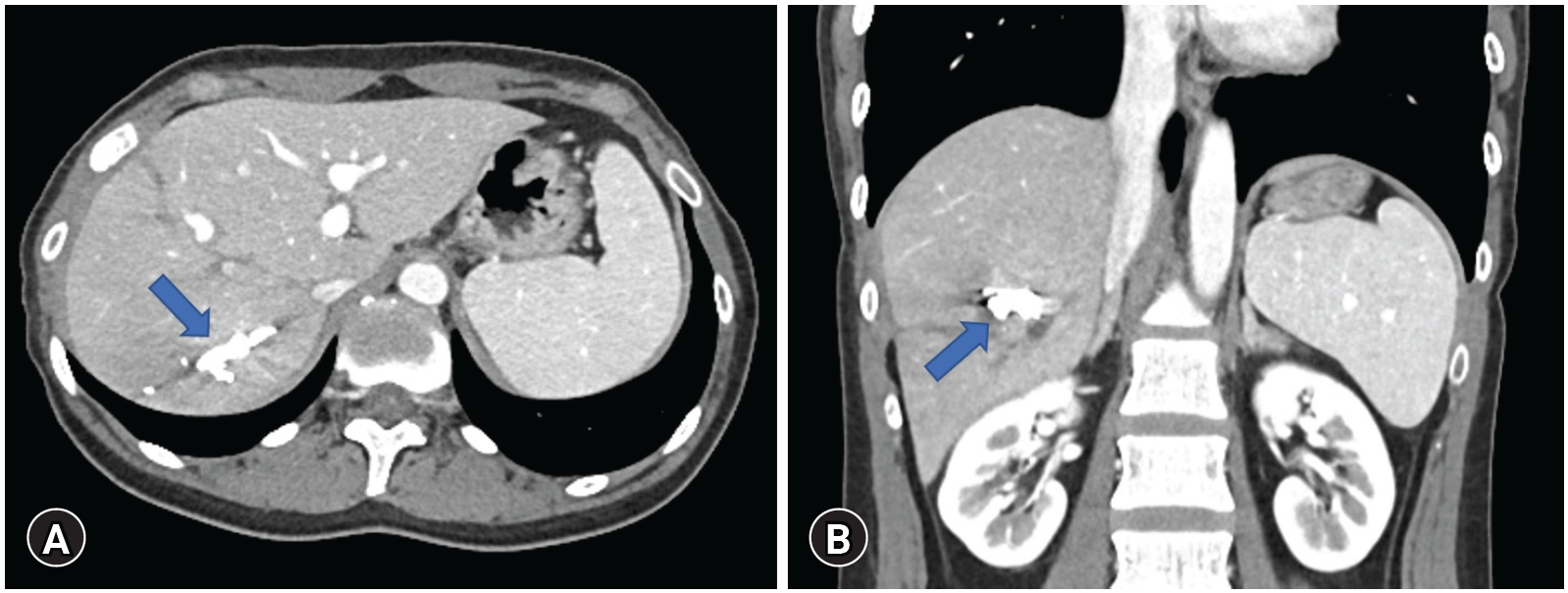
- On follow-up liver dynamic computed tomography performed 1 month after embolization, intraabdominal hematoma was decreased, the posterior branch of the right portal vein was sufficiently embolized, and no bleeding sign or liver parenchymal necrosis was observed (Fig. 3). Additionally, the patient’s aspartate aminotransferase/alanine aminotransferase were 599/550 U/L in the initial laboratory test, with the highest measurements obtained the next day at 857/802 U/L. The levels gradually decreased to 35/125 U/L after a week.
CASE REPORT
- The liver is the most commonly injured abdominal organ following blunt abdominal trauma. However, mortality from hepatic injury has declined over the last several decades. Richardson et al. [2] proposed that the reasons for the decreased mortality from hepatic trauma over the past 25 years are improved results with gauze packing and reoperation, use of arteriography and embolization, advanced operative techniques for major hepatic injuries, and decrease in the surgical treatment of hepatic venous injuries [1,2]. Additionally, the current approach to hepatic trauma has evolved to nonoperative management in more than 80% of cases [1]. Recently, a more extensive series of angiography for control of hepatic hemorrhage has been reported with increasing success, with the identification and control of bleeding rates ranging from 68% to 87%. Therefore, angiography and embolization or stenting are considered to be very useful adjunctive techniques in stable patients and are being managed nonoperatively [3].
- Hepatic arterial injury from blunt hepatic trauma is a common cause of massive hemorrhage, but significant bleeding from the portal venous system is rare because the portal venous pressure is usually low. In addition, portal vein injuries are generally associated with severe injuries affecting adjacent organs that often require surgical treatment, such as gauze packing, vessel ligation, and venorrhaphy [4–6]. As such, angioembolization enables nonoperative management of arterial bleeding in blunt traumatic liver injury, but portal vein injury suitable to performing PVE is very rare. PVE is a preoperative treatment commonly performed to increase the volume of the remaining liver in patients undergoing major liver resection. It is a safe and effective method for inducing selective hepatic hypertrophy of the non-diseased portion of the liver and may thereby reduce morbidity and shorten hospital stays after resection [7].
- In our patient, we decided to perform nonsurgical radiologic intervention because her vital signs were stable. If we decided to operate regardless, damage-control surgery, including gauze packing and reoperation, would have been performed and would have led to several postoperative complications, such as prolonged use of the mechanical ventilator, prolonged hospital stay, and even poor prognosis. Additionally, conservative treatment without intervention in this patient who with grade IV liver laceration accompanied by capsule injury, massive hemoperitoneum and active bleeding in the portal vein could worsen the condition even led to death.
- According to our experience, several conditions are necessary in performing PVE in patients with intrahepatic portal vein injury. First, the most important condition is stable vital signs. Next, the patient must be cleared of any other organ injuries requiring surgery. Furthermore, unlike elective PVE, the intervention for trauma patients is urgent. An experienced radiologist must be present for accurate identification of trauma lesions and determination of the portal vein puncture site. Anatomic variants of the portal vein are uncommon but, when present, are important to recognize because they may have profound implications for PVE [7]. Finally, the surgical team should be prepared to perform emergency surgery immediately if the procedure fails.
- In summary, our report demonstrates that PVE could be a good alternative treatment for portal vein injury in patients with stable vital signs.
DISCUSSION
-
Ethical statements
Informed consent for publication of the research details and clinical images was obtained from the patient.
-
Conflicts of interest
The authors have no conflicts of interest to declare.
-
Funding
None.
-
Author contributions
Conceptualization: KHL; Project administration: SHC; Visualization: all authors; Writing–original draft: SHC; Writing–review & editing: all authors.
All authors read and approved the final manuscript.
ARTICLE INFORMATION

- 1. Piper GL, Peitzman AB. Current management of hepatic trauma. Surg Clin North Am 2010;90:775–85. ArticlePubMed
- 2. David Richardson J, Franklin GA, Lukan JK, et al. Evolution in the management of hepatic trauma: a 25-year perspective. Ann Surg 2000;232:324–30. ArticlePubMedPMC
- 3. Badger SA, Barclay R, Campbell P, Mole DJ, Diamond T. Management of liver trauma. World J Surg 2009;33:2522–37. ArticlePubMedPDF
- 4. Sundarakumar DK, Smith CM, Lopera JE, Kogut M, Suri R. Endovascular interventions for traumatic portal venous hemorrhage complicated by portal hypertension. World J Radiol 2013;5:381–5. ArticlePubMedPMC
- 5. Park CY, Yeom SR, Cho HM. Life-threatening traumatic rupture of an intrahepatic portal vein. Trauma Image Proced 2017;2:13–4. ArticlePDF
- 6. Majdalany BS, Khaja MS, Sanogo ML, Saad WE. Percutaneous glue embolization for recalcitrant iatrogenic portal hemorrhage. Diagn Interv Radiol 2018;24:385–7. ArticlePubMedPMC
- 7. Madoff DC, Hicks ME, Vauthey JN, et al. Transhepatic portal vein embolization: anatomy, indications, and technical considerations. Radiographics 2002;22:1063–76. ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- Portal vein embolization following arterial portography for the management of an active portal bleeding after blunt liver trauma in a cirrhotic patient
Romain L’Huillier, Bénédicte Cayot, Jean Turc, Laurent Milot
CVIR Endovascular.2024;[Epub] CrossRef
- Figure
- Related articles
-
- Blunt abdominal trauma resulting in pancreatic injury in a pediatric patient in Australia: a case report
- Gastric necrosis after gastric artery embolization in a patient with blunt abdominal trauma: a case report
- Nonoperative management of colon and mesocolon injuries caused by blunt trauma: three case reports
- Azygos and right superior intercostal vein injury secondary to blunt trauma: a case report
- Inhalation injury after a landmine explosion: a case report
 KST
KST

 PubReader
PubReader ePub Link
ePub Link Cite
Cite